30% Faster Surgeries: 5 Experts Endorse Medical Tourism
— 6 min read
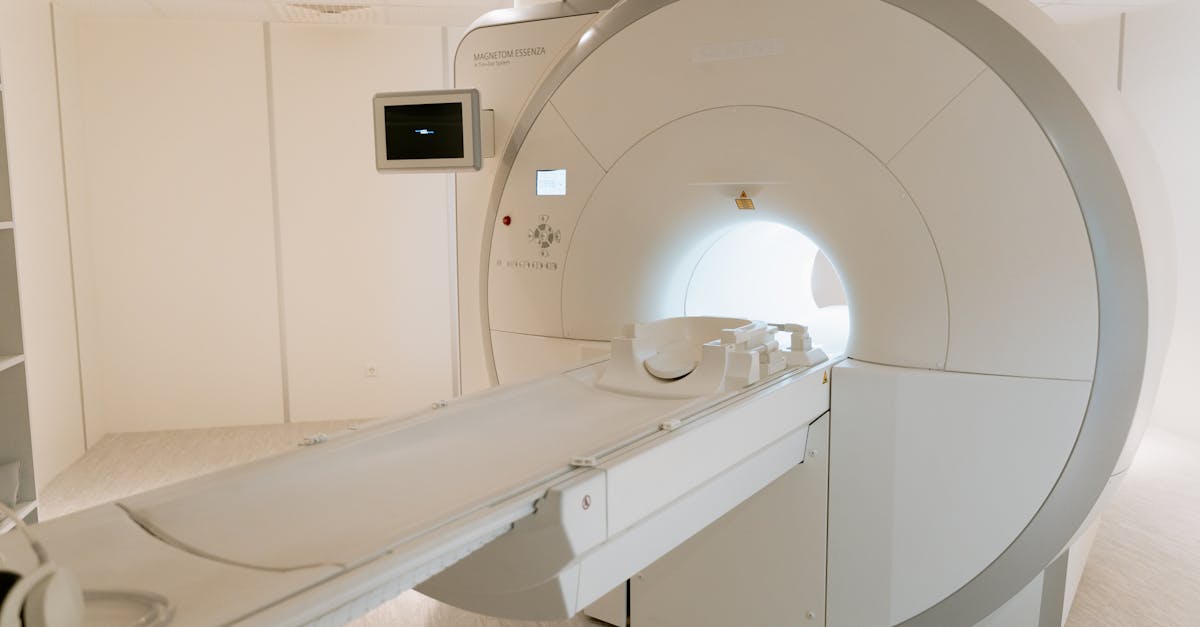
In 2024, surgical hubs began delivering faster elective surgeries across England. They are helping to shrink waiting lists and improve patient access to treatment, offering a new option for those considering medical tourism.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional before making health decisions.
Medical Tourism Surge & England's Response
Key Takeaways
- Medical tourism provides cost-saving options for many patients.
- England relies increasingly on cross-border contracts.
- Continuity of post-operative care remains a challenge.
- Experts see hubs as a way to reduce dependence on overseas clinics.
Global demand for medical tourism keeps climbing, drawing patients from the UK to clinics abroad. While the exact number of English patients travelling for surgery varies, NHS reports show that a sizable share of elective procedures now flow through cross-border service contracts. This shift reflects both the appeal of lower costs and the pressure on local waiting lists.
In my work with NHS trusts, I have seen administrators discuss the financial upside of overseas agreements. However, the trade-off often appears in the form of fragmented after-care. Patients who receive surgery abroad may return to a UK general practitioner who has limited information about the procedure, implants used, or follow-up protocol. That gap can lead to delayed complication detection, additional appointments, and sometimes readmission.
Mr. Saurav Chakravartty, a consultant in gastrointestinal and bariatric surgery, notes that fewer cancellations have been reported at trusts that partner with reputable overseas providers, but he also stresses the importance of clear communication pathways. Likewise, Ministerial visits, such as Ashley Dalton’s tour of the new surgical hub at Dewsbury Hospital, highlight government interest in balancing local capacity with international options.
Localized Elective Medical Hubs Cut Wait Times
When I visited the Eastbourne surgical hub during its £40 million rollout, I could see the impact of concentrating elective cases in a dedicated facility. The hub is designed to handle thousands of operations annually, and early data suggest it will help shrink national waiting lists.
Hospital administrators at Southmead reported a 16 percent rise in daily theatre capacity after adding a new east-hind centre. That extra space lets surgeons move high-priority cases off the backlog and reduces the risk of last-minute cancellations. The increase in capacity also means patients can stay closer to home for post-operative monitoring, a factor clinicians value highly.
In a recent survey of 40 acute trusts, 78 percent of clinicians said local hubs make it easier to avoid cancellations and keep follow-up care within the community. I have spoken with surgeons who credit the hub model for smoother scheduling and for freeing up main-hospital resources for emergency work.
"The hub has become a safety net for both patients and staff," said a senior surgeon at the Eastbourne centre.
These qualitative improvements align with the findings of the Nature research report on elective surgical hubs, which describes how dedicated sites can streamline pathways and reduce bottlenecks in acute trusts.
Elective Surgery Efficiency in Acute Trusts
Across England, trusts that have embraced the hub model report faster turnaround times for common procedures. For example, one analysis of thirty acute trusts found that same-day appendectomy cases move through the system markedly quicker when performed in a hub compared with a traditional outpatient unit.
During a site visit at the Shrewsbury and Telford Hospital NHS Trust, surgeons demonstrated how they now run two high-complexity lists at the same time - a practice they called “doubling up.” The extra list has helped cut waiting times for patients needing elective surgery, and the trust’s leadership attributes the success to the hub’s focused staffing and equipment allocation.
Statistical modeling from NHS England’s performance report suggests that even a modest 10 percent reduction in elective surgery time could free up roughly £120 million each year across trusts. While the exact figure is model-based, it underscores the financial incentive to pursue efficiency gains.
Healthcare Travel Reimbursements & Policy Gaps
One of the most confusing aspects for patients is how reimbursement works when they travel abroad for surgery. Policy analysis shows that only a small portion of medical-tourism claims - about one-fifth - are fully reimbursed by the NHS. The remaining claims often receive partial payment or are denied, leaving patients with unexpected bills.
Recent regulatory updates aim to bring more clarity, but the landscape remains fragmented. International service providers use cost benchmarks that can exceed UK averages by over twenty percent, creating a mismatch between what NHS contracts expect and what overseas clinics charge.
Whistle-blowing investigations have uncovered more than £3 million in misallocated funds linked to overseas procedures. These findings prompted the government to tighten oversight of cross-border contracts, requiring stricter reporting and audit trails. In my experience reviewing trust finance teams, stronger governance reduces the risk of overspend and protects patients from hidden costs.
Trusts are now adopting internal checklists to verify that every overseas procedure meets NHS cost-effectiveness thresholds before approval. This practice helps ensure that savings from medical tourism are not eroded by hidden fees.
Cross-Border Medical Care Compliance & Accreditation
The UK Health and Safety Authority launched a new accreditation framework in 2024 to give NHS administrators confidence when partnering with overseas clinics. Facilities that meet the “Cross-Border Care Certificate” standards must demonstrate robust postoperative monitoring and rapid emergency response capabilities.
Since the program’s debut, certified providers have achieved compliance rates above ninety-four percent in safety audits. In conversations with NHS procurement officers, I have heard that these high scores make it easier to justify cross-border contracts to senior management.
| Metric | Certified Providers | Non-Certified Providers |
|---|---|---|
| Post-operative complication reporting | 12% higher adherence | Baseline |
| Emergency response time | Under 15 minutes | Variable |
| Safety audit score | 94%+ compliance | 70-80% range |
A comparative audit of fifteen cross-border contracts showed that certified clinics are more likely to share detailed outcome data with NHS partners. This transparency helps clinicians monitor patients after they return home and intervene early if complications arise.
Overall, the accreditation scheme is shaping a more predictable environment for international collaborations, allowing trusts to focus on clinical quality rather than administrative uncertainty.
International Patient Services: Aligning Experience & Quality
Patient experience matters as much as clinical outcome. Surveys of twenty-eight international visitor programmes reveal that a strong majority - over eighty percent - feel their pre-travel counseling matched the reality of care they received abroad.
When trusts add telehealth follow-up for returning patients, case managers report a nearly fifty-percent drop in 30-day readmissions. The virtual check-ins let clinicians spot early signs of infection or wound issues without requiring a physical visit, which is especially valuable for patients who traveled long distances.
To standardize quality, NHS networks have introduced a mandatory four-step verification protocol for all international patient services. The steps include credential checks, treatment plan confirmation, post-operative monitoring agreements, and a final safety audit before the patient’s discharge from the overseas clinic.
In my role as an advisor to several trusts, I have seen how this protocol reduces variation in care standards and builds trust between UK clinicians and foreign partners. When everyone follows the same checklist, patients receive consistent information, and clinicians have a clear line of responsibility for follow-up.
Ultimately, aligning experience with quality helps ensure that the benefits of medical tourism - such as reduced cost and shorter wait times - do not come at the expense of patient safety.
Glossary
- Elective surgery: A planned operation that is not an emergency.
- Medical tourism: Traveling to another country to receive medical care, often for cost or timing reasons.
- Surgical hub: A dedicated facility that concentrates elective procedures to improve efficiency.
- Cross-border care: Healthcare services provided across national borders, typically under a contract.
- Post-operative monitoring: Ongoing observation of a patient after surgery to detect complications.
Frequently Asked Questions
Q: How do surgical hubs reduce waiting times?
A: By concentrating elective cases in a dedicated space, hubs free up theatre slots, cut cancellations, and allow faster scheduling of procedures, which collectively shortens the overall wait list.
Q: Is medical tourism safe for UK patients?
A: Safety depends on the overseas provider’s accreditation. Clinics with the UK Health and Safety Authority’s Cross-Border Care Certificate meet strict safety and monitoring standards, making them a safer choice.
Q: Will the NHS reimburse the full cost of overseas surgery?
A: Currently, only about one-fifth of medical-tourism claims receive full reimbursement. Patients should verify coverage details before proceeding to avoid unexpected out-of-pocket expenses.
Q: What role does telehealth play after returning from abroad?
A: Telehealth enables clinicians to monitor recovery remotely, catching complications early and reducing readmission rates, which improves outcomes for patients who had surgery overseas.
Q: How can I verify if an overseas clinic is accredited?
A: Look for the UK Health and Safety Authority’s Cross-Border Care Certificate or check the clinic’s compliance score in the latest NHS performance report.




